[et_pb_section admin_label=”section”]
[et_pb_row admin_label=”row”]
[et_pb_column type=”4_4″][et_pb_text admin_label=”Text”]
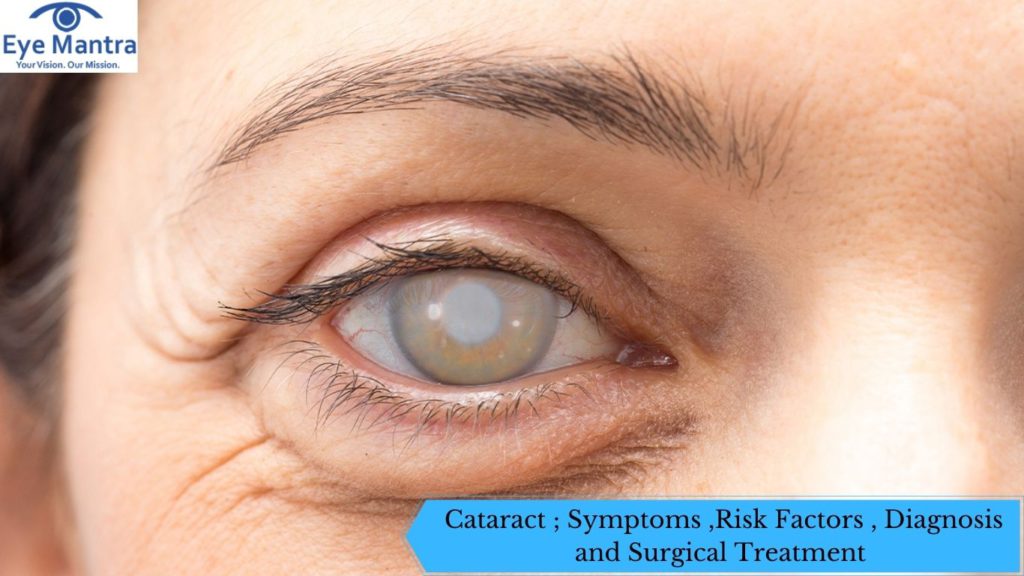
A cataracts is eyes related lens abnormality characterized by decreased transparency and increased cloudiness that eventually prevents it from sending clear images to the retina. It is becoming one of the leading causes of reversible visual impairment and blindness globally where the number of cases are expected to increase with an ageing population. The World Health report estimates approximately 20 million people to be bilaterally blind with less than 3/60 visual acuity in the better eye and about 100 million eyes with cataract causing a visual acuity (VA) of less than 6/60. The condition is found to be more prevalent in populations with lower socioeconomic status and in developing countries owing to insufficient surgical facilities that have posed as a major challenge for ophthalmologists on public health stance. Though the incidence of cataract blindness has been speculative but the estimates do suggests < 6/60 VA in 25 million eyes globally and about 3.8 million people in India becoming blind from cataract every year.
Symptoms of cataract
Natural lens of the eyes is a crystalline biconvex structure that refracts (bens) the light rays to produce a clear passage for our vision. Any modification, aggregation and precipitation of crystalline proteins are, Therefore considered detrimental to the main mechanisms underlying the cataract development. There are many subdivisions in a full classification, and these can be helpful in ascribing different levels of symptoms to a particular sub-type of cataract.
- Cortical cataracts:
- Light scatter from localized opacities and disruption of smooth light transmission.
- Difficulty in reading
- Problems with glare when driving
- Uncomfortable to sunlight in winters when the sun is considered to be low on the horizon
Additional effects common to the developing world includes
- Compatibility with daytime activities due to constriction in pigmented iris.
- Difficulty in night driving.
- Nuclear cataracts:
- Reduction in colour intensities
- Gradual reduction in contrast
- Difficulty in recognizing faces
- Difficulty in seeing golf balls or car number plates
- Reading is often surprisingly good for the Snellen level of acuity.
Additional effects common to the developing world include difficulty in working at fields during dusk.
- Subcapsular cataracts:
- Difficulty in daytime driving
- Difficulty in reading
- Less trouble at low light levels when pupils become dilated
Additional effects common to the developing world are characterized by visual disabilities as sunlight can become particularly bright to the condition.
Risk factors of cataract:
Cataract formation is considered to be mostly a multifactorial disease that develops with their specific etiologies and varies with the type of cataract, patient’s lifestyle or visual requirements. As new lens fibres continue to be laid down in the crystalline lens without replacing the existing ones, their optical homogeneities are maintained by several interdependent factors responsible for its microscopic structure and chemical constituents.
Adult-onset of cataract is primarily age-related (or senile). It is defined as cataract occurring in people >50 years of age that are unrelated to any known mechanical, chemical, or radiation trauma. The mean age of presentation for cataract is estimated to be 62.46 years in India where 70% of the study population has shown VA <20/200. Similar ages at presentation were also reported in Africa (66.5 years) and Canada (73.4 years) with studies from Nepal showing 11.5% of patients being operated for cataract as blind at presentation. The estimates clearly reflect its severity with progression resulting in reduced light transmission from the gradual accumulation of yellow-brown pigment within the lens. Moreover, Several structural changes to the lens fibres also add disruption to their regular architecture and arrangement of the fibres that are otherwise necessary to maintain optical clarity. Such conditions may further aggravate the underlying symptoms of senile cataract through the specific mechanisms of oxidative damage, abnormal migration of lens epithelial cell, elevated calcium or deficiency of glutathione.
A number of metabolic conditions such as diabetes mellitus have also been linked to the accelerated rates of cataract development. A poor control of diabetes mellitus is usually associated with non-enzymatic protein glycation, oxidative and osmotic stress resulting in several systemic and ocular complications including vision loss. Such individuals develop cataracts approximately 20 years earlier and might undergo cataract surgery for visually significant cataracts at a much younger age. Other metabolic conditions such as hypocalcaemia, Wilson disease and myotonic dystrophy may also increase the incidence of cataract in patients with pseudo-exfoliation syndrome and atopic dermatitis. Also, Ischaemic ocular conditions such as pulseless disease, thromboangiitis obliterans and anterior segment necrosis have contributed quite significantly to the cataract formation.
Extrinsic factors, on the other hand, has been widely associated with the variability in cataract formation from the prevailing socio-economic and geographical differences. This has been defined by the condition of malnutrition, acute dehydrating diseases at a young age, and exposure to excessive ultraviolet rays. In many developing countries, cataracts are still common in young adults which have been frequently associated with the treatment of their atopic disorders. This includes systemic, inhaled or topical use of corticosteroid in a dose – duration-dependent manner and use of several other drugs involving phenothiazines, miotics, amiodarone and statins. Blunt trauma along with perforating injuries, ionizing radiation, infrared radiation (to which glassblowers are frequently exposed) and microwave radiation can also lead to cataract formation where alkali burns are more likely to be severe than their acid injuries.
Diagnosis :
Patients are evaluated for visual impairment and other symptoms along with concomitant eye diseases that could potentially influence the surgical plan or visual outcome. Such an assessment can be done subjectively according to the patients’ perception or by visual acuity measurements that are recorded for both far and near distances. Analysis of the intraocular pressure, the lacrimal apparatus, eye alignment in the orbita, motility and pupillary function becomes helpful for planning surgery and providing a prognosis of the patient’s visual function. Slit-lamp biomicroscopy is performed to examine such abnormalities in the eyelids, lashes, cornea, anterior chamber, pupillary dilatation along with the hardness of cataract. Detailed fundus examination through a dilated pupil is used for evaluating the status of the lens, macula, peripheral retina, optic nerve and vitreous humour. Supplement tests such as contrast sensitivity, glare disability and ocular wavefront testing for visual aberrations can help to identify the cause and level of severity of visual symptoms. Testing with a potential acuity meter, laser interferometer or scanning laser ophthalmoscope involves projecting an image onto the retina through relatively clear regions of the lens to predict the visual acuity following cataract surgery. If necessary, other ancillary tests could also be performed including colour vision or visual field measurement, optical coherence tomography, fluorescein angiography and B‑scan ultrasonography.
Surgical treatment :
Deteriorating visual function from cataracts requires a restoration of the transparency of the optical pathway through replacement of the clouded crystalline lens with an IOL of appropriate refractive power. Current surgical techniques achieve these goals with precision, reproducibility and safety owing to our ability to measure the optical parameters of the eye, advanced technologies to remove the cataract and continuing advances in IOL design. All modern techniques are variations of extracapsular cataract surgery, in which most of the surrounding clear lens capsule is preserved to permanently support the IOL. Zonules (microscopic ligaments) are attached and inserted circumferentially onto the lens capsular equator to suspend and support the lens. After removing the firm lens nucleus and softer surrounding cortex, IOL is then placed within the vacated capsular bag where it lies anterior to the remains of the cleared capsule.
In order to measure the results of cataract surgery, it is necessary to define the outcome. This has been explained by the WHO Prevention of Blindness Programme in terms of visual acuity, which can be assessed with full spectacle correction (“best vision”), or with available correction (“functioning vision”). Poor outcome is defined as <6/60.13, the borderline outcome as <6/18 to 6/60 and a good outcome as 6/6–6/18. As the period from surgery of acuity measurement also affects the results, it should therefore be standardised for an individual situation so that trends over time can be reviewed. Studies from developing countries are usually divided into clinical trials/selected series, long term population-based studies and routine hospital-based data. The results from clinical trials and individual series have been good with poor outcome occurring in less than 5% of the cases, unlike the routine hospital-based reports and long term population-based studies.
Naturally poor acuity experienced by patients following surgery affects the demand for cataract surgery by the community. And there seems little doubt that the poor results due to lost aphakic spectacles and surgeries by inexperienced personnel under inadequate conditions are still having a negative impact on people’s perceptions of cataract treatment.
The best way to treat your eyes is to visit your eye care professional and get your eyes checked regularly. He will be able to assess the best method of treatment for your eye ailment.
Visit our website Eyemantra.To book an appointment call at +91-8851044355. Or mail us at eyemantra1@gmail.com.Our other services include GLAUCOMA SURGERY, Specs Removal, Smile Eye Surgery , and many more.
Related Articles :
[/et_pb_text][/et_pb_column]
[/et_pb_row]
[/et_pb_section]